Sleep Apnea
Did you know that...
- Many dentists are trained to evaluate and help treat snoring and obstructive sleep apnea (OSA)?
- Dr. Pickard has been practicing dental sleep medicine for over 15 years, and is an American Academy of Dental Sleep Medicine qualified dentist?
- Sleep disorders, including OSA, affects an estimated 18 to 30 million adults in the US, and people with OSA can stop breathing up to 100 times per night? (National Sleep Foundation and American Academy of Dental Sleep Medicine, 2017)
- It is estimated that 1% - 10% of children in the US have obstructive sleep apnea? (American Academy of Family Physicians, 2004)
Providing our patients with beautiful healthy smiles is just as important as supporting our patients’ overall health and well-being. As an added service within our practice, Dr. Pickard is seeing family members of patients who have sleep and airway concerns.
What is sleep apnea?
Sleep apnea is a condition in which your breathing stops periodically during sleep, as many as 20-30 times per hour. Each time you stop breathing in your sleep, the resulting lack of oxygen alerts your brain, which temporarily wakes you up to restart proper breathing. The constant wake-sleep, wake-sleep cycle prevents those with sleep apnea from achieving deep sleep, resulting in a constant drowsy feeling during the day.
What are the risk factors for sleep apnea?
- Enlarged tonsils and adenoids in children often related to inflammation due to frequent upper respiratory infections
- Overweight/obesity
- Family history of OSA
- Structurally narrow airway passages
- Smoking tobacco
- Drinking alcohol
- Use of sedatives/tranquilizers
- Health history of stroke, brain tumors, neuromuscular disease, and heart disorders
What are the signs of sleep apnea?
- Snoring
- Mouth-breathing
- Gasping or periods of no breathing while asleep
- Frequently waking up at night
- Restless during sleep
- Bed wetting
- Fatigue & lack of energy during the day
- Moody/irritable
- Poor concentration & worsening school performance
- Behavioral problems such as ADHD
- Clenching/grinding teeth at night
- Morning headaches
- Additionally, in adults, OSA is also associated with chronic acid reflux (GERD), polycystic ovarian syndrome, diabetes, and menopause
What are the risks of not treating sleep apnea?
- High blood pressure
- Heart disease
- Stroke
- Diabetes
- Chronic acid reflux (GERD)
- Increased risk of workplace and driving accidents
How is sleep apnea treated?
Weight management program, treatment of allergies and upper respiratory infections, and other health conditions associated with OSA, quitting smoking and drinking alcohol. These are important health conditions that should be treated first by your primary care provider.
Enlarged tonsils and adenoids in children: An estimated 85% of children with sleep apnea have enlarged tonsils and adenoids, which is often treated effectively with a tonsillectomy and adenoidectomy.
Continuous Positive Airway Pressure (CPAP) is the gold standard for the treatment of sleep disorders.
For those that do not tolerate CPAP well, other options are available, such as:
- Custom Oral Mandibular Advancement Devices: There are different types of devices depending on the region of airway constriction. A thorough sleep evaluation is necessary in order to prescribe the device that is most appropriate.
*It is important to note that although many people report positive results from their mandibular advancement devices, also called “snore guards,” statistics show that about 1/3 of people that try oral mandibular advancement devices receive no therapeutic effect.
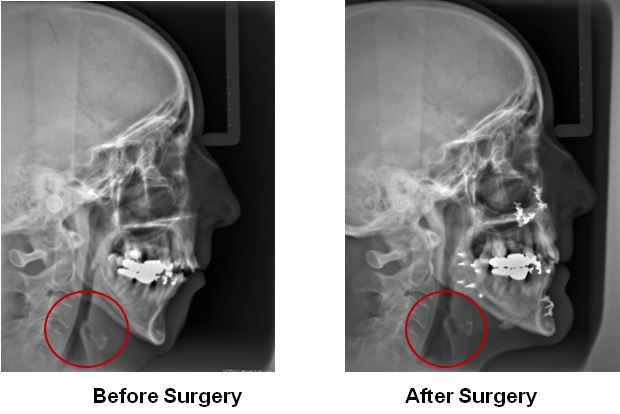
- Oral Surgery in conjunction with orthodontic treatment to advance the lower jaw.
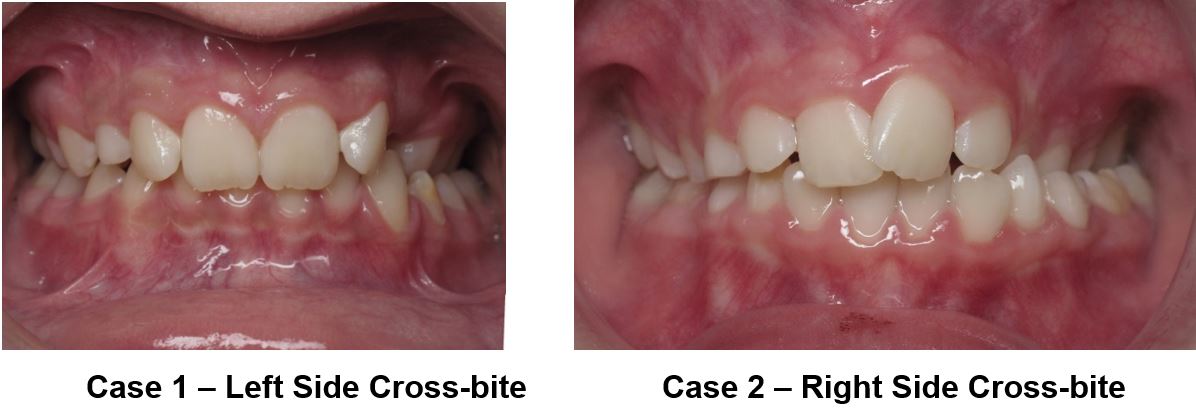
- Rapid Palatal Expansion (RPE): Orthodontic appliance to expand the upper jaw: For a small percentage of children, a narrow upper jaw may contribute to upper airway constriction, which also often manifests in poor fit and function of teeth, including excessive crowding and a cross-bite. A cross-bite is when the upper teeth incorrectly fit on the inside of the lower teeth, as shown below.
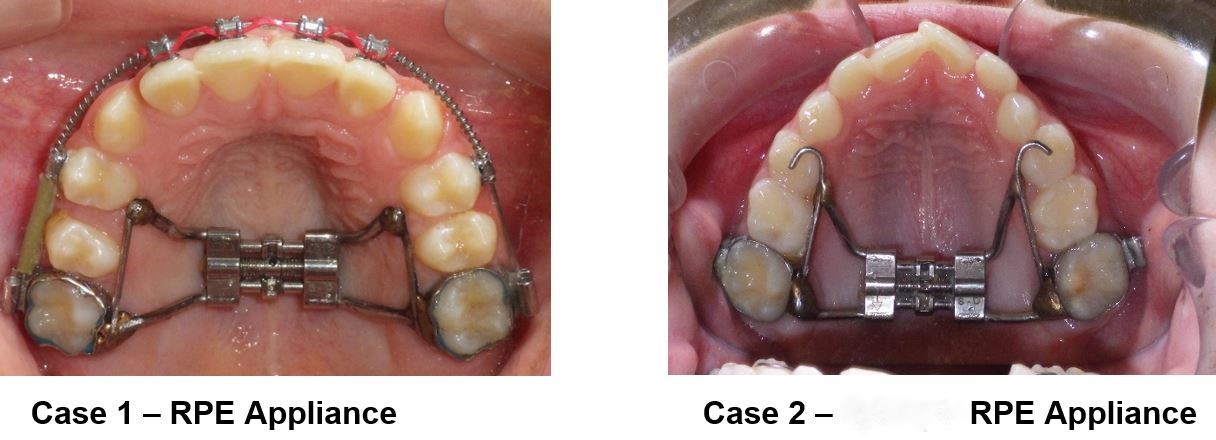
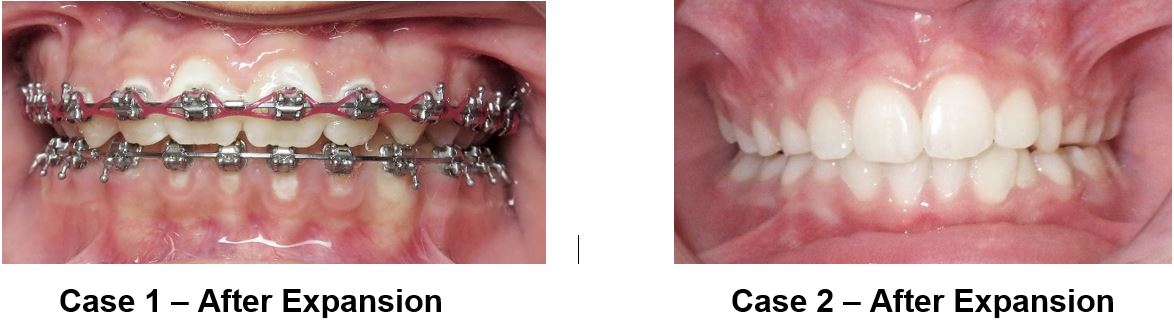
These children benefit from the expansion of the upper jaw, called Rapid Palatal Expansion (RPE), as shown below.
The upper jaw is made up of two bones on either side with a suture that runs down the middle of the palate. Research indicates that the ideal time to achieve the most predictable results for an RPE appliance is between the ages of 8 – 12 because those two bones are not fused together at that age and children are in a rapid phase of growth and development making the body more responsive to treatment. The RPE applies some tension to those bones, and the bone responds by growing new bone. The body is pretty amazing, isn’t it? By the late teenage years, the upper palate bones fuse together making a solid suture, and any expansion at this point typically requires surgery.
Treatment with an RPE takes about 6 months, and with good patient compliance, it predictably corrects cross-bites of the teeth and increases upper airway space.
Unfortunately, this technique does not work on the lower jaw. Research shows that it is not possible to expand or make the lower jaw grow. Why? Because the lower jaw is one solid bone and applying tension to the bone is not going to grow the jaw, but rather, simply move the teeth through the bone.
Questions?
Please contact our office for more information regarding sleep apnea and how a dental sleep medicine may be able to help you.
References
American Academy of Dental Sleep Medicine. http://www.aadsm.org/
American Academy of Family Physicians (2004). Sleep Apnea in Children. Retrieved from http://www.aafp.org/afp/2004/0301/p1159.html
Chan, j., Edman, J, and Koltai, P. (2004). Obstructive sleep apnea in children. American Academy of Family Physicians. Retrieved from www.aafp.org/afp
Huynh, N.T., Desplats, E., Almeida, F.R. (2016). Orthodontics treatments for managing obstructive sleep apnea syndrome in children: A systemic review and meta-analysis. Sleep Medicine Review. Doi: 10.1016/j.smrv.2015.02.002
Sutherland, K., Vanderveken, O. M., Tsuda, H., Marklund, M., Gagnadoux, F., Kushida, C. A., & Cistulli, P. A. (2014). Oral Appliance Treatment for Obstructive Sleep Apnea: An Update. Journal of Clinical Sleep Medicine : JCSM : Official Publication of the American Academy of Sleep Medicine, 10(2), 215–227. http://doi.org/10.5664/jcsm.3460
Ready to get started with a new smile?
Select an office for your free consult below